Scientists in the US have developed the first hand-held optical scanner that can be used for the early detection of breast cancer. The device, made by Britton Chance of the University of Pennsylvania and colleagues, is intended to be a complement to traditional breast screening methods, such as mammograms, and could be commercially available within the next few years (Rev. Sci. Instrum. 77 064301).

It is now thought that 1 in 10 women will develop breast cancer. Although highly efficient scanning techniques, such as mammography — which take X-rays of the breast — exist, these can be uncomfortable and not everyone has access to them. A portable device that both patients and doctors could use would overcome these problems while also providing women at high risk of contracting the disease with a way of regularly examining themselves.
The device consists of a plastic box measuring about 10 cm by 10 cm with a circuit containing two light-emitting diodes (LEDs) and one diode, amplifiers and a microchip. The LEDs emit light in the near-infrared region of the spectrum between about 650 and 900 nanometres. Since water and fat do not absorb light at these wavelengths very much, the light is able to penetrate as deep as 5 cm into the tissue.
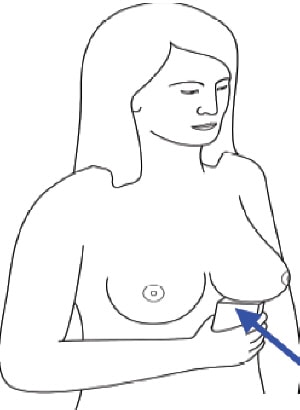
The device is then scanned over the breast and can detect a growing tumour by changes to the absorbed signal: when the scanner passes over the tumour, more light is absorbed because there are more blood vessels in growing tumours than in surrounding healthy tissue. So the idea is that the device monitors a fall in intensity in tumour regions. The scanner can also be connected to an audio device so that it emits a loud beeping noise when it reaches a tumour and a quieter one when it passes over healthy tissue. This information can be saved on the microchip for a doctor to analyse later.
The device has already performed well in a small pre-clinical trail on 100 women, correctly detecting cancer in 92% of the patients. This is comparable to MRI and better than mammograms says the researchers.
However, unlike mammography, and other such techniques that detect anatomical changes, the scanner detects physiological changes that occur in the earliest stages of breast cancer. Detecting breast cancer early on is crucial so that it can be treated before it has time to spread to other parts of the body. The device is also suitable for women under 40 who have denser tissue that is difficult to penetrate using conventional techniques. The team is now working on securing funding to develop a clinical prototype and hopes to commercialise the device within three years.