Researchers in Israel have invented a new type of breath test for detecting lung cancer in patients using sensors built with gold nanoparticles. Although the analysis of breath particulates is not a new tool in cancer diagnosis, this is the first technique that could detect cancer without the need to pre-treat the exhaled breath, say the researchers.
Lung cancer accounts for more than a quarter of all cancer-related deaths with an estimated 1.3 million people dying from the condition worldwide each year. Breath testing is an established, non-invasive method that works by linking “volatile organic compounds” (VOCs) with specific forms of lung cancer. The drawback of this method at present is that it requires collecting samples and analysing them using techniques such as mass spectrometry and infrared spectroscopy.
Tiny gold nuggets
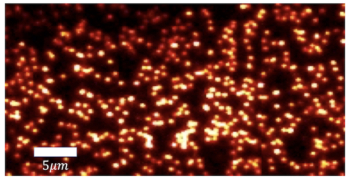
Hossam Haick at the Israel Institute of Technology and his colleagues have now developed a new device for detecting cancer in breath, which could provide an almost instant diagnosis of a patient’s health, they say. At the heart of the new device is a carbon-based sensor with embedded gold nanoparticles.
When a patient breathes into the device, particulates in the breath accumulate on the carbon layer and the sensor swells, pushing the gold nanoparticles further apart, which, in turn, alters the resistance of the film. Each type of particulate has a unique effect on the resistance, which can be measured by having a current flow through the sensor. “The user gets a figure on the device’s display panel that indicates whether the person is healthy or has cancer,” says Haick.
Having inserted the new sensor into a breath-test device, the researchers then carried out a series of tests for calibration purposes. By recruiting 96 volunteers – 40 lung cancer patients and 56 controls – the team built up a catalogue of VOCs based on the electrical signals that were present in the breath of lung cancer sufferers but not in the breath of controls.
Skip the trials
Haick and his team are currently testing their new device on a wider range of volunteers in order to consider the impact of factors like diet, alcohol and genetics. Moreover, in a break from the convention in medical innovation, the researchers claim that full clinical trials may not be necessary to take this new technology to a stage where it is hospital-ready. They believe instead that they could prove the device’s accuracy using a series of “artificial mixtures” of particulates that could simulate cancerous and healthy breath.
Tony Cass, a biomedical engineer at Imperial College, London, sees promise in the new technique but he has his reservations about the idea of bypassing clinical trials. “It has the potential, but will need a lot more clinical validation before it becomes accepted,” he says. Cass warns about the danger of oversimplifying real-life cancer diagnoses. “The use of ‘synthetic’ breath is a good way to test some aspects of the device but the nature of the approach using sensors arrays and chemometrics requires evaluation in complex – i.e. real patient – samples,” he adds.
In addition to lung cancer, this new device has also been used to promising effect in the diagnosis of other diseases including renal failure, Haick told physicsworld.com. Cass also agrees that the device has the potential to become a flexible addition to the medical toolkit. “It may find earlier use in monitoring a patient’s response to treatment and could be useful in ruling out other diseases that may present similar symptoms to lung cancer in the early stages such as chronic obstructive pulmonary disease,” he says.
This research appears in the latest edition of Nature Nanotechnology.