
Dutch researchers have developed a workflow involving 3D virtual and 3D-printed models that may change how complex spinal surgeries are managed. Using this new technique, surgeons were able to repair a 12-year-old girl’s severe and debilitating spinal deformity.
In a technical report, first author Peter Pijpker and colleagues from University Medical Center Groningen outline how they constructed a 3D virtual model and 3D-printed model of the spine of a patient with a severe deformity. Clinicians used the 3D models to both preoperatively plan a challenging surgical treatment for the patient and intraoperatively guide the operation (World Neurosurg 10.1016/j.wneu.2018.07.219).
The 3D virtual planning and 3D printing technique was feasible for the surgery of a complex spinal deformity and may help improve clinical outcomes in the future, the authors noted.
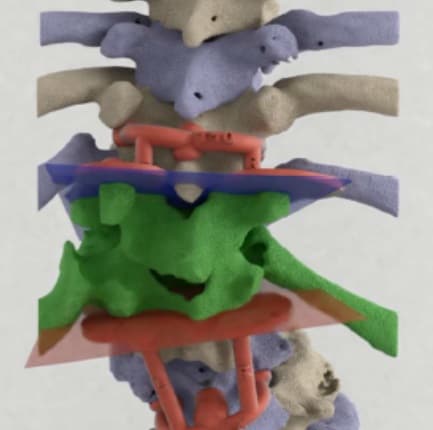
“The [3D-printed] templates and bone models provided valuable guidance during the osteotomy in the severely deformed anatomy,” they wrote. “Moreover, the surgeons report that studying the 3D anatomy in a multidisciplinary team facilitated the surgical procedure due to enhanced spatial orientation.”
Accurate planning
Pedicle subtraction osteotomy is a technically demanding procedure for repairing spinal deformities and is associated with a risk of major complications. The surgery is particularly challenging when dealing with severely deformed spines.
“Operations of the severely deformed spine call for new, more precise methods of surgical planning,” the authors wrote. “[Three-dimensional] technology can give rise to new possibilities for the surgical planning of spinal deformities.”
In a recent case, Pijpker and colleagues applied 3D technology not only to facilitate the surgical team as they planned the best course of action, but while they performed the operation as well. The case centred on a 12-year old girl with a combination of bone diseases — skeletal dysplasia and severe congenital kyphoscoliosis — that required the expertise of specialists from several different fields for surgical treatment.
The group began by acquiring MRI and CT scans of the patient’s spinal cord. Next, they segmented and reconstructed these CT scans and then created a 3D virtual model of the spine using 3D-modeling software (Mimics Innovation Suite, Materialise). Examining the 3D virtual model, they were able to plan the ideal way to complete the surgery — allowing them to prevent the patient’s spinal deformity from progressing any further and minimize the risk of future neurological deficit.
To guide the procedure itself, the researchers 3D printed the virtual model of the patient’s spine, and they additionally 3D printed individualized guiding templates that fit directly onto the bone. The 3D-printed templates helped direct the surgical chisel during the procedure and also ensured the spine would maintain its position while the surgeons were cutting away pieces of bone.
The production cost of the 3D-printed spine was approximately Euro 154, and the image segmentation and template design took the 3D printing specialists a full day of work to complete.
Successful correction
With the 3D-printed spine and guiding templates at hand, the surgical team was able to successfully resect the spinal deformity and close the separation. The young patient left the hospital eight days after surgery without any neurological deficit. Postoperative X-rays demonstrated the surgeons had properly corrected her spinal deformity.
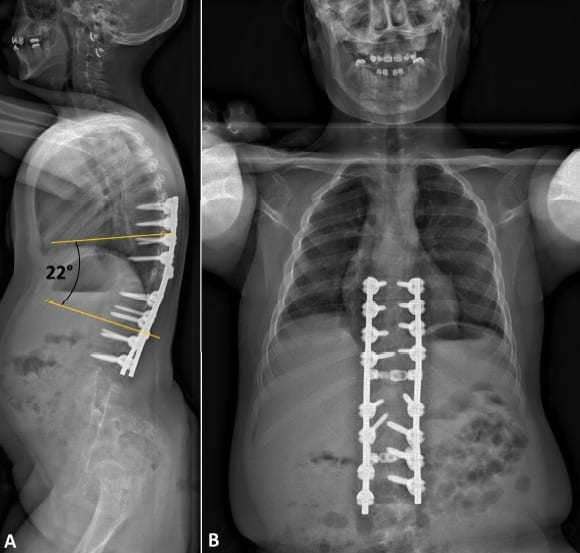
The authors described the following four key ways in which the 3D virtual model and 3D-printed models facilitated the operation:
- Provided insight of case-specific anatomy
- Helped in the identification of spinal bones during surgery
- Allowed for the visualization of deformed bones and their relation to the spinal cord
- Made sure the preoperative plan correlated precisely with the actual operation
One drawback of the technique was that intraoperative use of the 3D-printed models was limited to the first stages of the procedure. For the final step of the procedure, the surgeons had to temporarily replace the 3D-printed guiding templates with rods to further stabilize the spine. The investigators hope that subsequent template designs incorporate openings into which the surgeons can place the support rods. They also plan to assess the accuracy of using 3D-printed models for this surgery and the effect of doing so on patient outcomes, compared with other techniques.
“[Three-dimensional] virtual planning, 3D-printed spine models, and osteotomy-guiding templates have facilitated the performance of the osteotomy and may, in [the] future, contribute to safer spinal osteotomy procedures,” they wrote. “The presented method … might hypothetically reduce surgery time and preclude the need for intraoperative radiography, especially when combined with patient-specific drill guides.”
- This article was originally published on AuntMinnieEurope.com © 2018 by AuntMinnieEurope.com. Any copying, republication or redistribution of AuntMinnieEurope.com content is expressly prohibited without the prior written consent of AuntMinnieEurope.com.



