Malaria — a life-threatening disease and a serious global health problem — is caused by parasites transmitted by female Anopheles mosquitoes. The initial symptoms, such as fever, chills and headache, are not specifically associated with malaria, making accurate detection of malaria parasites important for diagnosis and treatment. Currently, however, diagnosis is often performed by visual analysis of blood slides for parasites — making its accuracy dependent upon the experience of the examiner.
Aiming to ease the intensive manual diagnosis process and improve its accuracy, a research collaboration from the USA, Thailand, India and the UK is developing an automated detection system for identifying and quantifying malaria parasites. The system provides reliable and standardized interpretation of blood films, as well as lowering diagnostic costs by reducing the required workload (J. Med. Imaging 10.1117/1.JMI.5.4.044506).
Malaria parasite detection system
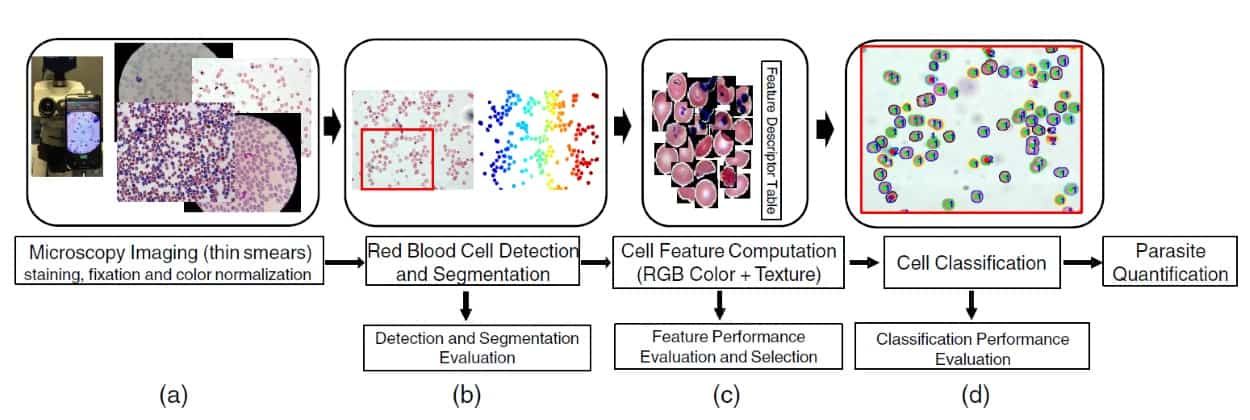
The automated system employs four main steps to detect the malaria parasite:
- Blood slides are prepared using staining and fixation; digitized images are then acquired using a standard light microscope and a top-mounted camera.
- A computerized technique detects and segments the red blood cells in the blood smear.
- The computerized technique characterizes the segmented red blood cells.
- Classification methods distinguish between infected and uninfected cells.
Despite unavoidable difficulties such as low image contrast, cell staining variations, uneven illumination, shape diversities, size differences and texture complexities during the detection and segmentation processes, the system can process about 100 cells/second. This means that it takes 20 seconds to examine around 2000 cells — a number that would take a specialized examiner between 10 and 15 minutes to assess.
The system characterizes segmented cells by colour (the red–green–blue model is suitable for determining the typical colour information of stained parasites) and by texture, to obtain information about changes in the appearance of the parasite during the different stages of its life.
Then, it uses classifiers such as SVM (support vector machine) and ANN (artificial neural network) to determine which cells are infected and which are not. To quantify the malaria infection, the system computes the infection ratio: the number of infected cells divided by the total number of cells.
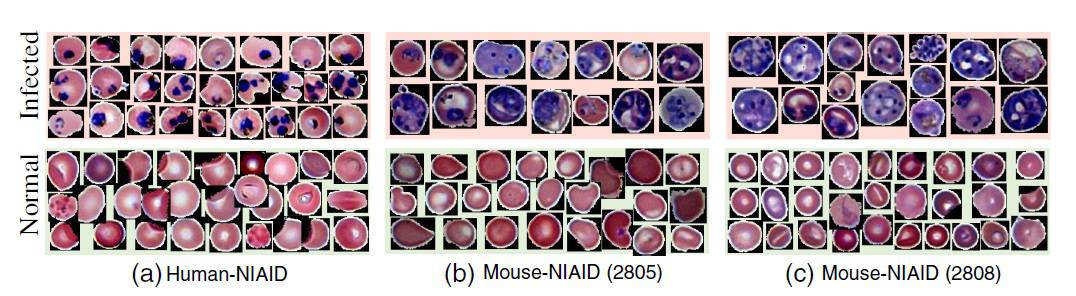
The researchers tested the automated system on human and mouse blood cells. They observed an absolute error of 1.18% between the actual infection ratio and the automatically computed infection ratio for human cells. For mouse cells, the automatic count correlated well with an expert examiner’s counts and with flow cytometry (used only for mouse cells).
This study presents the first robust system for automated detection of malaria infection in blood slide images from both humans and mice. The authors note that, importantly, the system could be implemented as a standalone smartphone app that’s well-suited for resource-poor malaria-prone regions.



