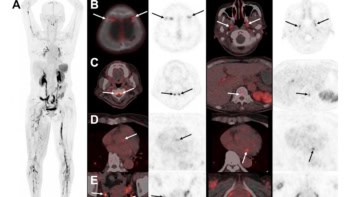
Dynamic MRI could better identify emphysema patients likely to benefit from invasive lung volume reduction surgery (LVRS), according to a study presented at the recent 68th Lindau Nobel Laureate meeting in Germany.
Emphysema results in reduced elasticity in lung tissue, causing it to remain hyper-inflated and preventing the fresh intake of oxygen with each breath. Surgery removes affected segments, providing more space for healthy lung tissue to expand in the thoracic cage during breathing.
Patients are typically selected for surgery according to CT scans and parameters measured by pulmonary function testing (PFT), such as the forced expiratory volume in one second (FEV1). Upon analysing their local patient population in Switzerland, however, researchers at the University Hospital Zurich found these criteria have limited predictive power.
“We had only 30-40% of patients with a treatment benefit,” said radiologist and first author Katharina Martini, who presented the research as a poster in Lindau. A proportion of the candidates for surgery also have cardiovascular disease, increasing the risk of complications in the operating theatre.
Martini and colleagues set out to assess the potential of dynamic MRI as a way to identify patients likely to have an improvement in lung function following surgery. They studied 39 patients referred for surgery, carrying out dynamic MRI scans one day before and three months following the procedure.
Patients also underwent PFT before and after surgery, providing a benchmark measure of lung function. Treatment benefit was defined in-house as a minimum increase of 30% in FEV1 following surgery.
The dynamic MRI scans comprised sagittal slices of both lungs acquired over two respiratory cycles during normal breathing. The researchers used an existing, commercially available balanced Steady-State GRE sequence, TrueFISP, on a 3T Siemens Skyra scanner. The resulting frame rate was 4 Hz. Patients were typically in the scanner room for five minutes.
Using the scans, the researchers then made a series of simple, geometric manual measurements of the lungs pre- and post-surgery. They included lung height, the anterior-posterior diameter of the thorax and the cross-sectional area of the lungs following full inspiration and expiration. Each measure was normalized by the patient height.
Complex measures and automated techniques not typically available on clinical scanners were avoided to make the approach as easy as possible to implement in routine clinical practise. “We wanted to keep it simple,” Martini told Physics World.
In a key finding, the researchers were able to demonstrate that the dynamic MRI data could measure changes in lung function following surgery. When analysed over the entire study cohort, statistically significant improvements in lung area in both lungs (pright=0.001, pleft=0.016) and the AP-diameter of the right lung (pright=0.003) on expiration were obtained following surgery.
The data also revealed that, based on the 30% FEV1 threshold, the pre-operative MRI measurements could predict a patient’s outcome following surgery. Using a receiver operating curve (ROC) analysis, the researchers found the pre-operative normalized total lung area on expiration was the most sensitive predictor. The parameter had a sensitivity of 86% and a specificity of 61%, corresponding to a pre-operative normalized lung area greater than or equal to 358 cm2.
Arguably, one drawback of the dynamic MRI approach is its significantly higher cost than the tests currently used in clinical practise. However, the benefits of avoiding unnecessary surgery in 60% of patients currently referred for the procedure still significantly outweigh the costs, Martini told Physics World.
The researchers hypothesize that MRI-derived patient selection criteria are likely to be most beneficial in addition to existing clinical criteria, rather than replacing them. Advancing the work, Martini and her colleagues are now investigating ways to combine the two sets of measures into a single score indicating a patient’s suitability for surgery.
The study was accepted for publication during the Lindau meeting and will appear in the European Journal of Cardiothoracic Surgery.