
Researchers in the US have used MRI-guided radiation therapy (MR-IGRT) to treat a tumour in the heart of a patient fitted with an implantable cardioverter defibrillator (ICD). The first successful procedure of its type on record, the technique highlights some challenges that need to be addressed in the future. The results will help the technique become more commonplace over the next few years as the clinical availability of MRI-linacs increases (Pract. Radiat. Oncol. 10.1016/j.prro.2019.02.003).
After ten years in development, linear accelerators (linacs) integrated with MRI scanners moved into the clinic in 2017. At Washington University School of Medicine (WUSM) in St. Louis, one application that has been found for the MRI-linac’s excellent soft-tissue contrast and real-time guidance is the treatment of cardiac tumours. Now, H Michael Gach and colleagues from WUSM, Barnes Jewish Hospital and Loyola University Medical Center outline one such procedure that was more complicated than the norm.
The male patient was admitted for stereotactic radiosurgery for a cardiac fibroma. The tumour was assumed to be the source of the patient’s ventricular tachycardia (accelerated heartbeat) for which an ICD had been implanted.
Non-invasive stereotactic cardiac radiosurgery — in which radiation is delivered in a single fraction — has been shown recently to be effective in patients with ICDs in reducing ventricular tachycardia events, but has so far been achieved without real-time image guidance. MR-IGRT involving multiple dose fractions, on the other hand, has been used to treat cardiac tumours, but not in the presence of ICDs.
“The motivation was that we needed to tackle the challenge of MR-IGRT in a patient with a nearby ICD so we can extend MR-IGRT to treating tachycardias using non-invasive stereotactic cardiac radiosurgery, in which the patient typically has an ICD or pacemaker,” says Gach.
The challenge of integrating an MRI scanner with a linac lies in avoiding or overcoming the interference effects that arise when both subsystems are operating at the same time. Researchers have achieved this by shielding the linac from the MRI’s strong magnetic fields and shielding the MRI from the linac’s radiofrequency fields.
The problem is, subjecting the patient to a magnetic field is a fundamental part of the imaging process, so the ICD cannot be similarly shielded. The proximity of the ICD to the planning target volume means that some irradiation of the device by the radiotherapy beam is inevitable too.
To ensure the safety of the procedure, the team employed a pre-operation checklist detailing the conditions that had to be met before the procedure went ahead. One of these conditions was that the ICD must be confirmed to be robust to the magnetic field strengths, field gradients, and radiofrequency energy absorption rates associated with the treatment.
The ICD was also required to be tolerant of the radiation dose that would unavoidably be delivered to the device. The vendor set an accumulated dose threshold beyond which it might suffer damage, but even below this level, the device had to operate in a limited-function mode to meet MRI and radiation safety guidelines.
First UK radiation treatment using MR-guided linac
Those conditions having been met, the most significant problems that the team encountered were the appearance of artefacts in the MR images acquired during the radiation therapy, and an image gating latency of up to half a second.
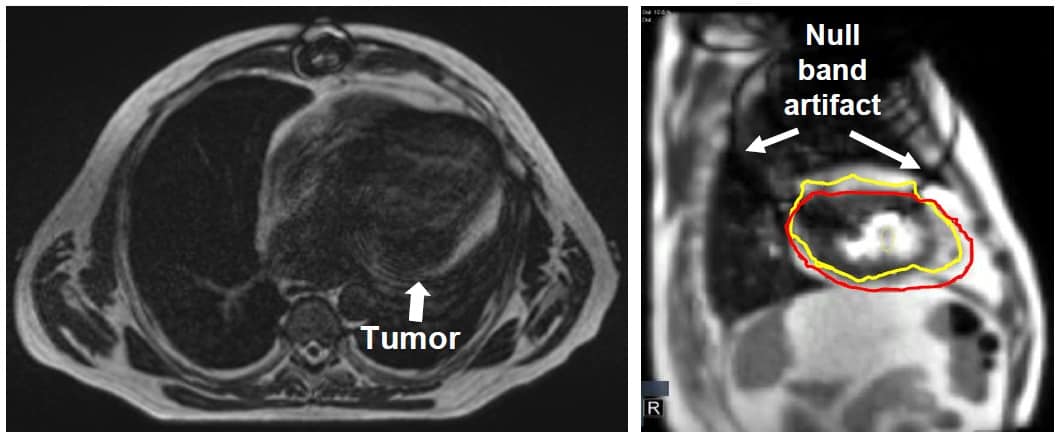
The “null band” artefacts were due to magnetic inhomogeneities associated with the ICD and showed up as dark bands intersecting the target area. The researchers note that these artefacts could be minimized under alternative MRI pulse sequences, but not without sacrificing signal-to-noise ratio. A different sequence could also help speed up the image acquisition process, reducing gating latency and sparing healthy tissue.




