Creating whole organs in the lab is a distant dream. Some experts think it always will be. But as innovations in 3D bioprinting begin to filter out of research groups and into the commercial and clinical worlds, less headline-grabbing advances could nevertheless prove significant, as Margaret Harris reports

In biomedical science there are dreams and there are realities. Here is one of the realities: right now, more than 5000 people in the UK need a new kidney. Over the next year, after a median wait of about 30 months, slightly fewer than half of them will receive one. The rest will continue to wait, but they cannot hold on forever: in 2016, 457 Britons died while waiting for a new kidney, liver, heart or lung. Another 875 were taken off the waiting list, mostly because they had become too ill to receive a transplant.
Build your own
Now here is one of the dreams: what if, instead of relying on scarce donated organs, scientists could quickly and cheaply build healthy new ones in the laboratory, with cells taken from the patients themselves as the raw material? For the past 15 years this dream has helped drive investment and research in an interdisciplinary field known as 3D bioprinting. The basic idea is to take principles from additive manufacturing – where three-dimensional objects are “printed” layer by layer according to a pre-programmed design – and apply them to challenges in tissue engineering. So, in a typical bioprinting experiment, researchers might fill a specialized 3D printer with liquid or semi-liquid “bioinks” containing living cells, and input a blueprint for a desired final structure. The printer’s nozzles will then scoot back and forth, extruding material line by line until a three-dimensional chunk of tissue (such as the human ear shown above) takes shape. Depending on the type of cells being printed and the goal of the experiment, the cells may then spend days or weeks in a controlled environment, or bioreactor, that keeps cells supplied with nutrients and stimulates them to develop into mature tissue.
The list of tissues printed by this method is already impressively long, and includes tumours, blood vessels and organ tissues, as well as simpler structures such as cartilage, skin and bone. Given these achievements, it is easy to see why many have speculated that bioprinting could one day stretch to creating entire organs. At this point, though, another reality intrudes. “People are saying, ‘Oh, we will be printing organs, we will live forever’,” says Gabor Forgacs, a biophysicist who co-founded the first commercial 3D bioprinting firm, Organovo, in 2007. “And of course, that’s what we also thought at the very beginning. But that’s wishful thinking. This is a beautiful field. I think it has incredible promise. But one needs to be realistic.”
Getting realistic
Fortunately, more realistic dreams are also available, short of printing whole organs for transplant. One of these dreams is that 3D bioprinting could make it easier and cheaper to develop new drug treatments. Innovation in this area would certainly be welcome. In the early stages of the standard “drug discovery” method, biomedical researchers test thousands of chemicals to determine their effect on cells or tissue samples. Only the most promising “hits” are marked for further study. Even after this weeding-out process, though, failure rates are high: of the tiny fraction of hits that make it as far as pre-clinical trials, barely one in 5000 are ever approved for clinical use. Late-stage failures, when compounds are found to be harmful or ineffective only after animal or human trials, are particularly expensive, contributing disproportionately to the average £1bn+ cost of taking a new drug to market.
Reasons for late-stage failures in drug development vary, but one contributing factor is that much of this work is done in 2D cell cultures. These systems are cheap, well-established and widely understood by researchers across medical science. The only trouble is that what happens in 2D slices of tissue is sometimes very different from what happens inside 3D mice or humans. The structures that form in 2D cultures are simple, and sheets of cells do not take in nutrients or expel waste products in the same way as clusters do. In the cheapest and quickest drug tests, the target cells are also isolated from other tissues, including those that exist alongside them in a living organism. “Cells in a two-dimensional configuration essentially don’t communicate with each other,” Forgacs says. “They are not revealing about a three-dimensional body at all.”
To create a more realistic, but still cost-effective environment for drug testing, some researchers have used 3D printers to create complex structures out of non-biological materials. Once printed, these objects act as a scaffold for cells to grow on, promoting more lifelike behaviour than is possible for cells grown in traditional 2D cultures. Start-ups such as the US-based firm 3D Biotek specialize in creating these 3D scaffolds for the medical-research market, and some established device manufacturers such as Germany’s GeSIM have developed 3D printers optimized for printing common scaffolding materials. More advanced applications of bio-compatible scaffolds include materials that mimic human cartilage. Such materials could potentially replace the “shock absorbers”, or menisci, in damaged knees, bridging the gap between metal or plastic replacement joints and fully biological substitutes.
Hardware and wetware
For purists, though, creating bio-compatible scaffolds is not true bioprinting, because the inks used are typically polymers rather than living cells. The distinction is more than just academic. “If you print with a substance that is not animate material, then at the end of the printing process you have a product – it could be a chocolate cookie, it could be a part of an airplane,” Forgacs explains. “It’s not so in bioprinting. There, the product comes about after an elaborate maturation process. The biological material has to do the work.”

Synthetic bioscaffolds are also of limited use for more complex types of medical research – including another prominent bioprinting dream, which is to create physiologically and anatomically correct cancerous tumours for ex vivo study. “Oncology research has been traditionally done either in 2D or straight into animal models,” says Hector Martinez, co-founder and chief scientific officer of Cellink, a Swedish bioprinting start-up. “If we can create 3D cancer-tissue models that replicate not only the cancer cells but also the surrounding tissue, we can better study how drugs penetrate into the cancer.” Better tissue models could reduce the number of animals used in medical research – “a fantastic goal” in its own right, Martinez says – and would also have clinical applications. For example, tumours printed from a patient’s own cells could enable physicians to develop drug-treatment regimes tailored to attack that specific tumour, rather than generalized from tests on other cancers of a similar type.
Moving from biocompatible structures to fully biological ones introduces several novel technical challenges. “The key criteria are to minimize the damage to cells while they are being printed, and to form a stable three-dimensional structure after printing,” says Wei Sun, a biomedical engineer at Drexel University in the US and co-founder of SunP Biotech, a bioprinting start-up. The problem, he observes, is that these two criteria frequently clash. Many bioinks are a mixture of living cells and hydrogels, which are highly absorbent networks of polymers such as gelatin or alginate. The hydrogels help to protect the cells from excessive shear stress during the printing process, but they are structurally weak. Adding stronger synthetic polymers to the mix makes it easier to produce multi-layered structures that maintain their shape. In addition, physical and chemical methods of crosslinking, or “curing”, the hydrogels after printing can improve their mechanical strength.
Fundamentally, though, developing inks that can be readily extruded without damaging the cells, yet still form self-supporting features after they leave the nozzle, is difficult.
Sun and his colleagues have addressed this problem by developing printers that operate at different temperatures, so that users can tweak the viscosity of their bioinks by changing the ambient conditions. They have also built printers with multiple nozzles optimized for different types of cells and delivery media. Other groups have focused on non-extrusion-based bioprinters: in particular, one start-up, Poietis, has developed a commercial bioprinter that uses a laser to selectively evaporate bioinks from a substrate onto a platform. Regardless of the machines’ design, though, Sun hopes that by making bioprinters available commercially, more researchers will engage with the technology. “We need biologists to be with this community,” says Sun, who is editor-in-chief of the journal Biofabrication. “We need them to know how printing more complicated tissue structures can help them, so they are not just focused on 2D Petri dishes.”
In training
In Forgacs’ view, though, printers are not the only aspect of bioprinting that needs additional R&D. “A printer is a machine – a cool machine, but a machine,” he says. “Biology is much more complicated.” The hard part, Forgacs explains, is developing the right bioinks and then getting them to “do what they need to do to be living tissue”. He cites blood vessels as an example. Their shape is relatively simple, and larger vessels are big enough – 50 to 100 microns in diameter – for extrusion bioprinters to reproduce. Even so, a newly printed blood vessel cannot function like a natural one. Instead, its cells must first be “trained” to handle high fluid pressures in a bioreactor that mimics blood flow, so that they organize themselves in the correct way: endothelial cells on the inside, closest to the flow; smooth muscle cells next, to give the vessel elasticity; and then fibroblasts on the outside.

Martinez agrees that reproducing cellular-level structures is among the biggest challenges in bioprinting. “It’s not possible to reproduce nanometre-scale features directly with the bioprinter extrusion method,” he acknowledges. Instead, he and his Cellink colleagues are creating tissue-specific bioinks that can support the kind of micro-scale development Forgacs describes. “You have to use the biological system – if you give the cells the right stimulation, they know exactly what to do.”
Harnessing biology

One of the most important steps towards bioprinting tissues for implantation into living organisms is getting the printed tissue to form blood vessels. This process, known as vascularization, was demonstrated for the first time in 2014 by a team led by Jennifer Lewis, a materials scientist at Harvard University. She spoke to Physics World about that breakthrough and how research in the field has progressed since then.
Why is vascularization so important?
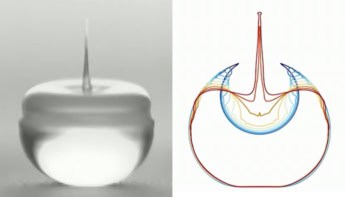
All cells need to be within a few hundred microns of a nutrient supply, so if you want to build true three-dimensional tissues – that is, tissues that are thicker than about half a millimetre – you need to embed a vascular network in the structure. This requires different materials to be co-deposited, and it also requires the ability to erode or erase one of those materials, leaving behind an open-channel network. What we did in 2014 was to demonstrate a full, multi-material bioprinting approach that allows you to simultaneously print cells, the extracellular matrix (ECM), and something we call a “fugitive ink”, which we use in effect to “draw” the vascular pattern of interest. After the tissue with the fugitive ink embedded in it has been constructed, we cool it down to about 4 °C. At that point, the ink becomes fluid, so we can just flush it away, leaving an open, cylindrical feature 100 to 200 microns in diameter that’s akin to what you would find in a vascular “highway” in your body.
What was the most difficult step in that process?
The actual printer design was relatively straightforward – we just needed to add additional print heads so we could simultaneously dispense multiple materials in a sequential fashion. The real problems were optimizing the material properties so that all of them would print appropriately; making sure that the extracellular matrix would foster cell proliferation and growth; and making everything compatible with the fugitive ink. We had to have different temperature-induced phase transitions, such that when we cooled the sample down, the cells that were suspended in the ECM surrounding the fugitive features remained intact and didn’t liquify. Otherwise we would have had a big puddle!
How has the field developed since then?
Our next goal was to create much thicker tissues – around 1 cm thick and inches on a side. In this case the cells we used were mesenchymal stem cells, which can be made to differentiate into things like bone, muscle or fat. We used the vasculature inside these thick tissues to feed in growth factor and other materials that not only kept the cells alive, but helped to program their differentiation. After 30 days, the cells had begun to turn into bone: they deposited their own collagen membrane and started to deposit minerals – calcium phosphate – that you would have in native, natural bone.
What’s next?
Our thesis is that bioprinting alone is not the best way to create human tissues – we need to harness as much biology as we can. That could mean starting with stem cells and programming them along the same paths as your body does, or it could mean allowing blood vessels that have been printed at a large scale to start to form tips and sprouts – capillaries, if you will – through a process called angiogenesis. We want biology to do as much of the heavy lifting as possible, because if you think about what it would take to print a kidney or a liver, we’re talking about tissue volumes that might range from a few hundred millilitres up to a litre. That’s a lot to print, and then the tissue has to function, which is a tall order as well.
An even bigger challenge, as we move forward, is to integrate that tissue into a host without triggering rejection or other immune responses, and have it not only function but be sustained. These are grand challenges, but it’s something that we’re working towards, and both we and others (such as Sangeeta Bhatia at MIT and Chris Chen at Boston University, and also Mike McAlpine at the University of Minnesota) have got steps along the way that we’re mapping out, one at a time.
A dream revived
This line of research raises the possibility of printing more complex tissues – initially as better testbeds for drug discovery and cancer research, but eventually as something that could be implanted into a patient. Erik Gatenholm, Cellink’s co-founder and CEO, is particularly bullish about bioprinted cartilage. The clinical need for replacement cartilage is strong: the tissue cannot readily repair itself once damaged, and worn-out knees are becoming increasingly common as populations age across the developed world. Cartilage’s structure is also relatively simple, and the material has been the subject of extensive bioink research. Gatenholm also points out that the nature of cartilage injuries is well-suited to incremental improvements in bioprinting technology. “If you have a partial tear of the meniscus, you’re going to want to come in and implant a partial repair to fix it,” he explains. “After that, we can study [the repair], and if it works really well you can go in with a bigger piece and a bigger piece. Eventually you replace the whole thing.”
The timeline for translating these and other bioprinting advances into the clinic is uncertain. Gatenholm predicts that patients could benefit from bioprinted cartilage or skin within the next 10 years. Sun says he can imagine a “major breakthrough” in bioprinted tissue models for cancer research in 5–10 years. And while Forgacs is pessimistic about the chances of bioprinting entire organs, the company he co-founded, Organovo, nevertheless announced in 2016 that it was shifting focus from pharmaceutical to therapeutic applications of its bioprinted liver tissue.
As with cartilage, Forgacs observes that even a small piece of bioprinted liver tissue could be clinically useful. “Somebody who needs liver transplantation typically has to wait quite a bit of time before a suitable donor is found, and they may die before such a donor is located at all,” he says. “But if you can implant a patch of tissue that would maintain somebody’s liver, giving it temporary functionality until a full donor is found, that would be fantastic.” As dreams go, it may not be quite up there with new organs arising like magic from lab-grown ooze. But for patients waiting for a transplant, it’s definitely a reality worth hoping for.