Innovation in proton therapy was front-and-centre at the ASTRO Annual Meeting, along with advances in other cutting-edge modalities – among them MR-guided adaptive radiotherapy, combined immunotherapy–radiotherapy approaches and stereotactic treatments for oligometatastic disease. Joe McEntee reports
While proton therapy has well and truly arrived as a mainstream treatment option in radiation oncology – there are currently 42 operational proton facilities in the US and a further 13 centres under construction – it’s evident that the clinical innovation is only just getting started when it comes to at-scale deployment of protons for the treatment of cancer. That’s one of the key take-aways to emerge from a dedicated conference session – Innovative Radiation Therapy Approaches: Benefits, Challenges, Global Perspective – at the ASTRO Annual Meeting in San Diego, CA, earlier this month.
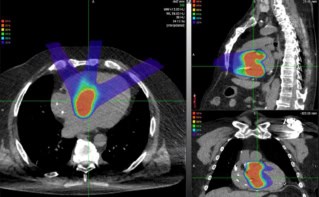
In terms of precision targeting, the case for proton therapy versus conventional radiotherapy is clear enough. Think similar tumour-killing properties as photons, but with markedly decreased dose to normal tissue. All of which helps the radiation oncology team treat tumours close to organs-at-risk (OARs), with the potential for decreased side-effects and complications along the way.
“Protons release all their energy at a point and then they stop,” explained James Metz, chair of radiation oncology at the University of Pennsylvania (UPenn) and executive director of the OncoLink cancer education service. That means no radiation dose beyond the target as well as far less dose deposited in front of the target compared with photon and electron irradiation.

As such, clinicians are able to target the tumour layer-by-layer with pencil-beam-scanned proton delivery. “We take a tumour, divide it up voxel-by-voxel into 5 mm3 volumes and take this pencil beam and treat [complex structures] spot-by-spot with absolutely no exit dose,” Metz noted. “Protons give us the opportunity to reduce dose to normal structures, to combine with chemotherapy and immunotherapy, and to increase [radiation] doses going forwards.”
Notwithstanding the ongoing roll-out of proton therapy systems across the developed world – clinical uptake is similar for the US, Europe and Asia, although currently there’s only one proton treatment centre in sub-Saharan Africa – it’s apparent that “gold-standard” evidence for the clinical efficacy of protons is still a work-in-progress. “We need to systematically evaluate the clinical potential and define it through rigorous science – quantifying the benefits versus investment,” argued Metz. “After all, substantial resource and infrastructure are needed to support a proton therapy centre.”
The evidence is coming – and sooner than later. A number of randomized phase III clinical trials are accruing data or have recently closed for diverse cancer indications (including lung, oesophageal, liver, head-and-neck and brain). Meanwhile, pragmatic trials are also accruing well and evaluating proton treatments in routine clinical practice for patients with breast cancer and prostate cancer.
FLASH the disruptor
Metz, for his part, is one of the clinical pioneers of proton therapy, having led the development programme for the Roberts Proton Therapy Center in Philadelphia – a facility that has treated thousands of cancer patients using protons since it opened its doors in 2010. Clinical innovation being what it is, however, attention is already turning to what’s being touted as the “next big thing” in particle therapy: FLASH proton therapy.
For context, FLASH is an experimental treatment modality that involves ultrahigh-dose rate delivery (above 60–80 Gy/s) of ionizing radiation (electron, photon or proton) over very short durations (less than 1 s). Preclinical studies have shown that FLASH radiotherapy is less toxic to normal tissues and as effective as conventional radiotherapy at destroying tumours. If broadly validated, FLASH treatment schemes therefore have the potential to revolutionize radiotherapy – such that higher doses could be delivered safely to tumours or established doses be given with reduced toxicity to OARs.
In short, FLASH proton therapy is shaping up as a future disruptor in radiation oncology, argued Metz, “bringing together biology and technology in new ways…and turning radiobiology on its head a bit”. The upsides are already coming into view. For starters, FLASH proton therapy could significantly compress radiation treatment times, such that radiotherapy becomes more like a surgical procedure.
Will ultrahigh dose rates transform radiotherapy in a FLASH?
That’s good news for the patient along several coordinates – opening a path to improved quality-of-life, reduced toxicity and side-effects, as well as much less time spent in the clinic. At a more fundamental level, FLASH irradiation can also trigger different immune pathways and gene expression, creating novel opportunities for drug and radiation combinations.
Yet while FLASH has the potential to upend treatment paradigms and many current assumptions about radiation delivery, Metz concluded on a cautionary note: “I would say FLASH proton therapy is not yet ready for prime-time…[and] not ready to be deployed further than a few highly resourced centres that can complete the appropriate research and clinical trials.”
Clinical innovation: it’s all about outcomes
Alongside the clinical opportunities afforded by proton therapy, the ASTRO session on Innovative Radiation Therapy Approaches covered plenty of other bases. Tamer Refaat, professor of radiation oncology at Loyola University in Chicago, Illinois, kicked off with a status report on MR-guided radiotherapy (MRgRT).
“The big deal [with MRgRT] is real-time adaptation,” Refaat told delegates. In other words, personalized, daily-adapted radiotherapy that’s based on real-time and on-table patient anatomy, allowing the clinical team to maximize dose to the target volume and minimize dose to OARs.
As for MRgRT innovations to watch, Refaat highlighted the commercial and clinical roll-out of cine-gating functionality to enhance the treatment of upper abdominal tumours on a single phase of breathing. “The radiation beam turns on whenever the target is within the tracking boundary and turns off when outside,” he explained (adding that the downside is longer time on the treatment table for the patient).

Incorporation of functional MRgRT into the MR-Linac workflow also came under the spotlight, with Refaat citing researchers at MD Anderson Cancer Center (Houston, Texas) among the early-adopters seeking to identify radioresistant tumour subvolumes and escalate dose to those subvolumes accordingly.
Another hot topic centred on the combined-modality synergies of integrating immunotherapy and radiotherapy cancer treatments. The speaker, Silvia Formenti, a radiation oncologist at Weill Cornell Medicine in New York, is one of the main-movers behind a paradigm shift in radiobiology, her efforts elucidating the role of ionizing radiation on the immune system while demonstrating the efficacy of combined radiotherapy–immunotherapy regimes in solid tumours.
Formenti highlighted the pivotal role played in this regard by the ImmunoRad Radiation Oncology-Biology Integration Network (ROBIN). A multidisciplinary R&D collaboration between US and European cancer centres, ROBIN is seeking to better understand the interaction of radiation therapy and the immune response – as well as nurturing the talent pipeline of early-career scientists into the field. Right now, noted Formenti, the bigger picture is clouded by “financial toxicity”, with the cost of immunotherapy proving prohibitive for most low- and middle-income nations – as well as many Americans.
The focus on collaborative clinical research was echoed by Stephen Harrow, a consultant clinical oncologist at the Edinburgh Cancer Centre in Scotland. In the final talk of the session, he discussed the application of stereotactic body radiotherapy (SBRT) for oligometastatic disease.
Post-pandemic, Harrow highlighted how the Scottish Oligomet SABR Network (SOSN), aided by £1 million of Scottish government funding, has enabled Scotland’s five cancer centres to offer a joined-up SBRT treatment service to patients across the country (not just the highly populated central belt encompassing Glasgow and Edinburgh).
The goal of SOSN, he explained, is to “build a network of physicians, physicists and radiographers so that we’re all agreed on patient selection [criteria for SBRT] and we have equity for patients across the country”. What’s more, he added, “the evidence is definitely building that you can influence patient outcomes with SBRT for oligomet disease.”