Focused ultrasound (FUS) provides non-invasive, targeted therapy for a wide range of clinical applications. Recently, FUS has proved effective at stimulating or inhibiting neuronal activity in both the central nervous system (CNS) and peripheral nervous system (PNS), offering the potential to replace existing neuromodulation therapies, which are either targeted but invasive, or non-invasive and non-specific.
To date, in vivo studies examining the physiological effects of FUS stimulation have only targeted structures in the CNS. Now, Columbia University researchers have demonstrated the first successful in vivo FUS stimulation of the PNS (Phys. Med. Biol. 63 035011).
“Neurostimulation of the CNS excites (or inhibits) many neurons, while with PNS stimulation, we are targeting either the axon or nerve body of a specific, well understood, nerve branch,” explained first author Matthew Downs. “FUS could be a powerful tool to target multiple nerve types including the vagus nerve, which has the potential to treat diseases such as epilepsy, depression and metabolic disorders.”
It’s also easier to deliver FUS to peripheral nerves, as the ultrasound does not need to pass through skull, which leads to energy loss and scattering. “If we can achieve similar effects by stimulating the peripheral nerves as we do the CNS, then the technique can be more easily implemented,” noted Downs.
Physiological response
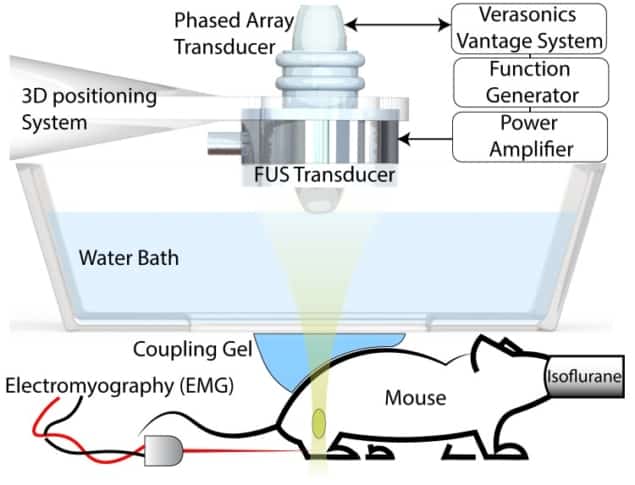
To demonstrate FUS stimulation of peripheral nerves in vivo, the researchers stimulated the sciatic nerve in anesthetized mice. They targeted the nerve using ultrasound imaging and stimulated it with a 3.57 MHz transducer. At the same time, they recorded electromyography (EMG) signals via needle electrodes placed into the tibialis anterior muscle, which is activated by sciatic nerve stimulation.
Preliminary experiments revealed a set of FUS parameters that successfully elicited EMG signals and observable muscle contractions. These included a 35-100% duty cycle (DC) and a stimulation duration of 0.8-10.5 ms. An 8 ms stimulation of the sciatic nerve typically produced a single EMG spike, and occasionally a second EMG signal, plus an electromagnetic field (EMF) artefact from the transducer. Reducing the stimulation duration to 0.8 ms at 100% DC (continuous wave) produced single EMG responses with reduced EMF noise.
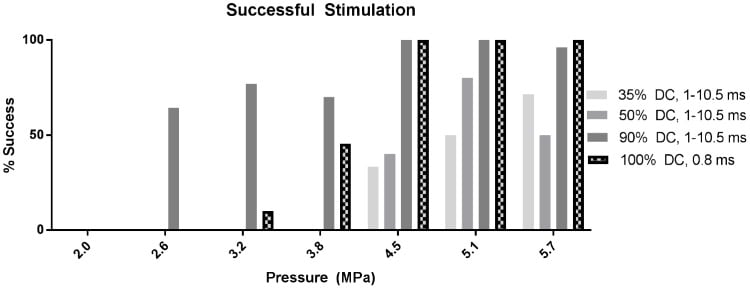
Varying the duration between 1 and 10.5 ms did not affect the latency (time between stimulation and response) or intensity of the EMG signal, thus the researchers combined results from this range. “From there, we wanted to see if we could achieve stimulation with a shorter duration, so we pushed the software to as fast as it could go, which turned out to be 0.8 ms,” explained Downs. “This was also an attempt to get as close as we could to normal electrical stimulation duration.”
Moving the FUS focal spot away from the sciatic nerve eliminated both observable muscle activation and EMG activity. To further verify that these effects were due to stimulation of the nerve, rather than the surrounding tissue, the researchers clipped the nerve downstream of the FUS target; this transection eliminated the EMG signal.
Comparing ultrasound with electrical nerve stimulation revealed that FUS could elicit comparable EMG spikes. The latency of the electrically stimulated EMG response (average 2.1 ms) was comparable to that of both the 0.8 ms and the 1-10.5 ms FUS stimulation groups. These findings suggest that FUS could serve as an alternative or complimentary treatment for peripheral nerve conditions currently treated with electrical stimulation.
Safety first
To assess the safety of this procedure, the researchers performed an open field test, in which they observed mice in a 30 cm2 box before and three days after FUS stimulation. The motion of the mice did not significantly change after stimulation and was similar to that of a control group – implying that FUS had not damaged the nerve or surrounding tissue.
They also monitored the time mice spent in the box centre and along its walls, to determine anxiety levels. The behaviour of the stimulated group was similar to the control and baseline groups, indicating that the FUS stimulation parameters used to elicit EMG responses are safe. H&E staining revealed no damage to the FUS stimulated nerves, reinforcing the safety of the technique.
Underlying cause
To determine whether FUS elicited a thermal effect, the researchers embedded thermocouples in an ex vivo mouse hind limb adjacent to the sciatic nerve. Stimulation at higher FUS pressures caused a 1.09°C increase in temperature – significantly lower than the 20°C increase shown previously to block nerves from firing.
They also measured the acoustic radiation force generated from the transducer and used this to determine the deformation at the focus. FUS parameters employed in this study generated a large enough displacement (up to 422 µm) to facilitate firing of an action potential that (according to prior studies) will elicit EMG activity. These in vivo findings agree with published ex vivo results stating that FUS excitation of the PNS is a mechanical, not thermal, effect.
The researchers are currently working to develop elastography-based targeting techniques for real-time monitoring of the transducer’s focal area to ensure accurate nerve targeting. They are also investigating whether cavitation is generated during stimulation, to further elucidate the mechanics of peripheral nerve stimulation. “We have also begun preliminary experiments with stimulation of human peripheral nerves using this technique,” Downs told medicalphysicsweb.



