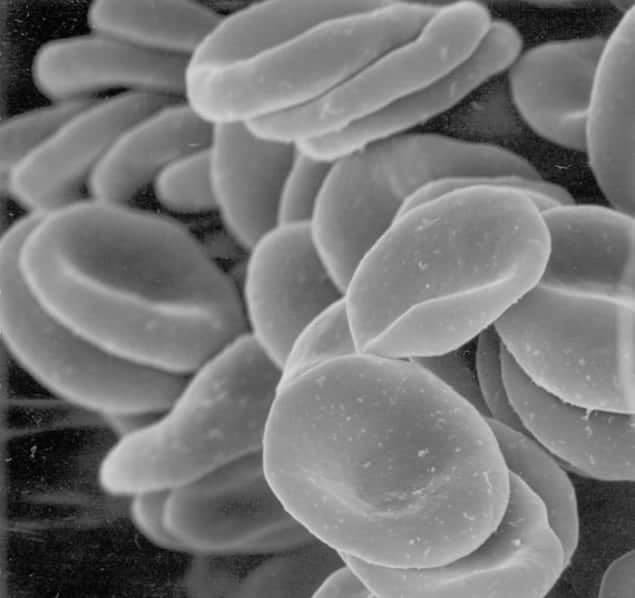
Physicists in France and the US claim to have discovered why red blood cells adopt asymmetrical “slipper” shapes in small blood vessels. If correct, the knowledge could be used to diagnose certain diseases that affect cell structure, although not everyone agrees with the researchers’ conclusions.
Red blood cells moving through large blood vessels normally adopt symmetrical parachute shapes. But for 40 years scientists have known that, in smaller blood vessels, the cells often lose their symmetry and take on a shape something like a lopsided slipper. Until now, no one has seemed to know the reason why.
Chaouqi Misbah of Joseph Fourier University in Grenoble, France, together with colleagues from there and the Georgia Institute of Technology in Atlanta, believe they have the answer. They modelled a red blood cell as a flexible membrane, ignoring the network of structural proteins, or “cytoskeleton”, contained within. They then calculated how the membrane adapts – in particular, how it resists bending – when it is pushed by a liquid flow.
Do slippers go with the flow?
The team’s model showed that, at lower flow speeds and when the membrane’s area is squeezed below a certain threshold, the symmetrical parachute shape becomes unstable and the red blood cell begins to look like a slipper. However, it also showed that neither the blood vessel size nor the membrane elasticity was a crucial factor. The researchers suggest that the blood cells evolved to take on the slipper shape so that they improve “flow efficiency” – in other words, so that they reduce the lag in speed between them and the liquid.
But Timothy Secomb, a physiologist at the University of Arizona, disagrees. He says that the model could benefit from a more realistic representation of red blood cell properties, and that the significance of the change in shape for flow efficiency is “overstated”.
“I would say that the flexibility of the red blood cell is important for reducing flow resistance in the circulation, and the slipper shape is just a consequence of that deformability, but does not serve any specific purpose,” he adds. “In reality, a wide variety of shapes are seen when multiple cells interact at normal hematocrit [red blood cell density] levels.”
Diagnosing infections
Still, Misbah thinks that his group’s model could be used to diagnose certain diseases that affect membrane rigidity, such as malaria. By comparing the shape of real cells to model predictions, they could tell whether the cells have been infected, he says.
The researchers are now planning to refine their model by adding the cytoskeleton, and to study the shape of red blood cells when there is a line of them in a channel. They predict that the cells will adopt alternating shapes, with one slipper pointing up, the next down and so on. “This will be the most efficient way for transport,” Misbah says. “Then we want to make a link between this shape transition and oxygen supply to tissues.”
The results are reported in Physical Review Letters.




