
With a single radiation treatment, a patient’s irregular heartbeat will be corrected; but there’s a catch. This particular patient inhales unevenly but exhales smoothly, presenting an uncommon challenge to the patient’s care team: as the patient breathes unsteadily, their heart moves irregularly, so healthy heart tissues will receive some unwanted radiation.
Nicholas Hindley, an Australian Fulbright scholar and PhD candidate at the University of Sydney’s ACRF Image X Institute, may have found a ready solution to this problem. He and his collaborators developed an algorithm that tracks the diaphragm – the predominant driver of internal organ motion during a radiation treatment – in real-time using low-energy X-rays. The tracking algorithm would help a patient’s care team irradiate affected regions of the heart and avoid healthy tissue without needing any specialized equipment, just a standard linear accelerator and some code.
Irregular diaphragm motion? No problem
Hindley is driven by the increasing global burden of cardiac arrhythmias – abnormal heart rhythms – and the growing demand for timely, inexpensive and non-invasive treatments like cardiac radioablation.
“There has been a recent flurry of activity in the medical physics community to develop safe and effective ways for treating abnormal electrical activity in the heart using radiotherapy,” said Hindley. “The technology required for real-time tracking of targets and organs-at-risk is available now, without the need for fancy, expensive equipment. We simply need to complement existing hardware with clever software.”
Hindley’s latest work, published in Physics in Medicine & Biology, uses simulation studies to demonstrate that the research team’s diaphragm-tracking algorithm, combined with the imaging capabilities of a standard linear accelerator-based radiotherapy system, can focus radiation to certain regions of the heart while avoiding others, all while a patient breathes.
The algorithm uses pictures obtained with four-dimensional computed tomographic (4D-CT) imaging to figure out how far the heart moves relative to the diaphragm’s motion. This respiratory motion model is then used to track the diaphragm, and thereby the heart, in real-time during treatment. The method accounts for motion of the heart’s substructures by applying a uniform margin before treatment.
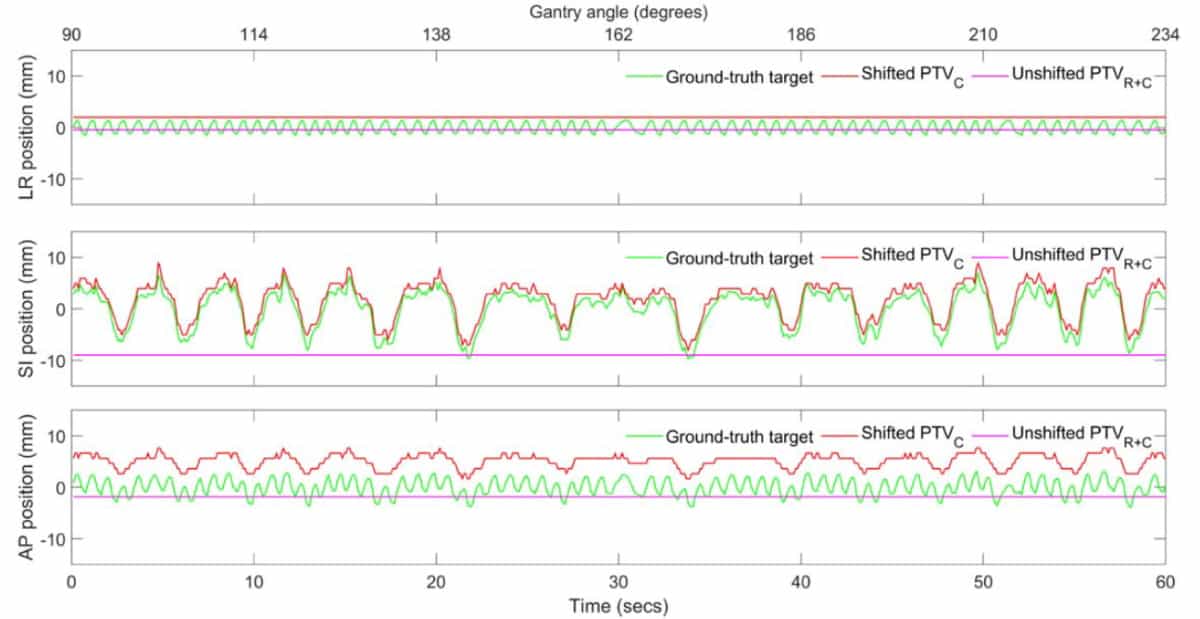
“There are many parameters within this method that may be tweaked, and the use of asymmetric margins is certainly one of them,” Hindley explains. “One could speculate that asymmetric margins may work well in an image-guided regime, since we know that the motion and deformation experienced by cardiac substructures is not uniform across the left–right, superior–inferior and anterior–posterior axes.”
Saving lives, improving quality of life
Hindley notes that their study is proof-of-concept as it uses digital phantoms developed by Paul Segars at Duke University. These digital representations of a patient, created using real patient images, are adjusted using biomechanical models so that researchers like Hindley can test their algorithms. Hindley plans to demonstrate the performance of the team’s code on real patient images using clinical trial data, anthropomorphic phantoms, or some combination of these.
One challenge Hindley foresees before the algorithm is implemented clinically is justifying the additional radiation dose the patient receives with X-ray imaging guidance. But he argues that the benefits outweigh the potential costs.
“This added radiation dose from X-ray imaging is miniscule when compared to the potential reductions in radiation with a more targeted approach,” Hindley says. “We hope tools like ours increase confidence for radiotherapy teams in treating these tricky targets. Over the long-term, we hope to facilitate the widespread adoption of cardiac radioablation, which has the potential to save or improve the quality of millions of lives every year.”



