Side effects of radiation therapy are a major concern to clinicians, even when using proton therapies that deliver highly conformal dose deposition. Therefore, it’s of clinical interest to develop methods that spare normal healthy tissue from toxic radiation. The application of short pulses of electrons at a high dose rate, known as FLASH irradiation, is one such method.
A few years ago, FLASH was shown to inhibit tumour growth with similar efficiency to radiotherapy techniques using conventional dose rates, while causing less harm to healthy tissue in vivo. However, the FLASH experiment used a prototype electron accelerator that is not available for clinical radiation treatments.
Previous work by another group showed that a linear accelerator can be tuned to deliver electron irradiation that meets FLASH specification, but researchers at the Institut Curie in France wanted to find out whether the same FLASH conditions could be achieved using protons from a clinical accelerator. The interdisciplinary team described the technological adaptations that they made to investigate FLASH in small animals (Int. J. Radiat. Oncol. Biol. Phys. 10.1016/j.ijrobp.2018.06.403).
“The idea was to change some of the parameters of the accelerator and test to see if you can produce proton beams that are inducing this very interesting FLASH effect,” says final author Ludovic De Marzi.
Developing the FLASH
FLASH irradiation requires the delivery of a high dose of protons in less than half a second. And to enable this protocol on their 230 MeV proton cyclotron at the Institut Curie, the team needed to use all of their cross-disciplinary skills to adapt the equipment.
“We have to use very different kinds of skills, radiation oncologists, medical physicists, computer scientists, electronic engineers, biologists,” says De Marzi. “So this was really difficult to have everyone talking and understanding the same language.”
The first challenge to address was the width of the proton beam. The beam had to be wide enough to irradiate the entire lung area in each swift treatment, but the accelerator’s beam was too narrow to cover the targeted murine pulmonary tissues.
To increase the width of the beam, the team put their heads together and developed a passive scattering system. They installed a high-density material, in the form of a thin, flat, lead foil scatterer, which deflected and expanded the beam to deliver a uniform proton dose to a 12 x 12 mm field size while keeping a very high dose-rate.
Dose accuracy
The team developed an electronic system to define the beam current to a high dose-rate and achieve FLASH conditions. But the dosimetry needed confirmation.
“It was difficult to monitor the dose because the detectors and monitoring chambers we usually use to count the number of protons do not really work at such a high dose rate and small radiation time,” explains De Marzi.
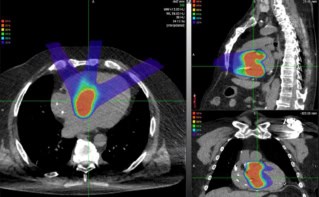
The spread-out Bragg peak (SOBP) used to deliver the total proton dose is classically obtained by rescanning and modulating the range of the proton beam at different energies. However, this approach was likely to increase the duration of irradiation and could spoil the FLASH effect. Ridge filters have been used previously to modulate beam range, and careful investigation proved that employing such a filter in the French team’s system would save time over conventional modulation.
The researchers tested a number of dose detectors at different proton beam levels, and compared the results with Monte Carlo simulations of the beam. They selected EBT3 Gafchromic films as the detectors that best coincided with simulations and used these as the reference.
Scaling for precision
“The most challenging part was to reproduce the accuracy we usually have for patients but at a different scale for small animals,” notes De Marzi. “This is far different from the way that we use the beamline and accelerator in clinics.”
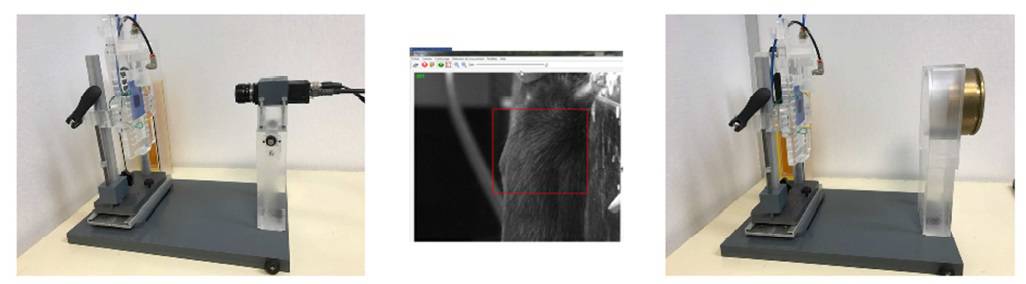
Precision was critical, and so the team developed a small-animal positioning system. An anaesthetized mouse was placed on an adjustable stand and images from a digital camera were compared with those from X-rays to enable accurate alignment with the proton beam. A validation study, where a mouse was readjusted several times, proved that the team could achieve sub-millimetre accuracy.
“We’re looking at lung fibrosis and expect the FLASH effect to be same for tumour as commercial load, but for tissues there should be protection,” says De Marzi, explaining that the group is patiently waiting for results from the in vivo study.