Post-traumatic stress disorder (PTSD) is a difficult condition to diagnose because scientists have yet to identify biological markers associated with the disease. Instead, doctors must rely on a patient’s descriptions of flashbacks, worry and emotional numbness when making a diagnosis. Now, researchers at the University of Minnesota Medical School have shown that measurements of the tiny magnetic fields created by brain activity can be used to identify genuine PTSD sufferers with high confidence – and without the need for patients to relive painful past memories.
The measurements are made using magnetoencephalography (MEG) – an established non-invasive technique that provides detailed information on the brain in almost real-time. This is done using superconducting quantum interference device (SQUID) sensors to measure the magnetic fields generated by currents flowing in and around neurons. However, these magnetic field signals are extremely weak – typically between about 10–14 and 10–13 Tesla – and are therefore easily overwhelmed by background magnetic noise. Although various techniques exist to reduce this noise, none are entirely satisfactory because they can also reduce the size of the signals produced by the brain itself.
The work by Apostolos Georgopoulos and colleagues builds on earlier investigations by the same group that demonstrated the potential of MEG to diagnose certain brain diseases from patterns of neuronal interaction (see “MEG differentiates functional brain disease“).
Interactions between signals
“The key idea that we have been using is that the essence of brain function is communication,” explains Georgopoulos. “You have a clean signal, but when you look at the interactions between these different signals, this is where we find the big difference between people with the disorder and healthy controls.”
The conditions studied previously, which included multiple sclerosis, schizophrenia and Alzheimer’s disease, have a clear pathology, Georgopoulos said. PTSD, on the other hand, is a purely functional brain disorder, which makes it particularly difficult to tell whether someone has the condition or not. This is where the MEG and the “synchronous neural interactions test” come into play.
Acquiring the MEG data is extremely easy and very safe, Georgopoulos said. “The acquisition itself is trivial: it takes about one minute to acquire the data. It is incredible how efficient the method is,” he commented. The equipment is, however, expensive to run because it must be cooled by liquid helium. Properly trained personnel are also needed to carry out regular maintenance and quality-control checks.
Subtle take
This latest study involved 74 patients with a diagnosis of PTSD who were known to the US Department of Veterans Affairs Medical Center in Minneapolis, and 250 similarly aged healthy controls recruited from the general population. Most of the patients (56) were taking medication designed to combat their anxiety.
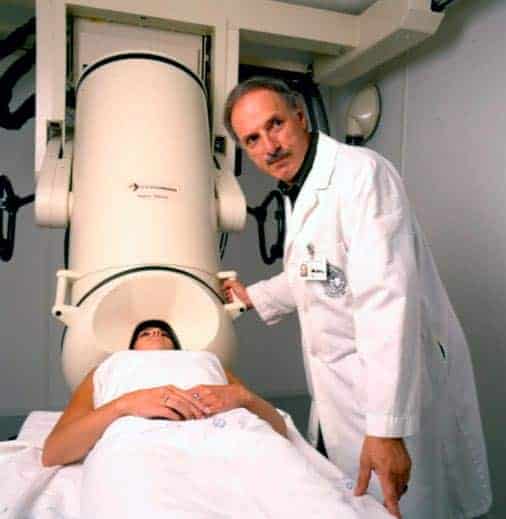
During the test, all subjects lay supine in an electromagnetically shielded chamber and focused for 60 seconds on a spot that was approximately 65 cm away from them. MEG data were acquired using a 248-channel axial gradiometer system lowered close to the head.
A “bootstrap-based” approach – in which the sample population being assessed was repeatedly altered at random – was used to classify subjects into two groups. The overall accuracy of the test came out at over 90% using this approach and all but two of the PTSD patients were identified correctly.
The method has “great clinical potential” as a diagnostic aid in cases of PTSD, according to Georgopoulos. Assessments of brain function are usually performed while subjects carry out a relevant task, so people claiming to have PTSD could be asked to view pictures or movies likely to trigger bad memories. With this MEG-based test, subjects merely stare straight ahead for one minute.
The benign nature of the test means that subjects are far more willing to return for repeat assessments, making it far easier to monitor the effects of therapy. Successive measurements could ultimately be used to predict the extent of remission and the likelihood of relapse in individual patients, Georgopoulos suggested.
The work is described in J. Neural Eng. 7 016011.



