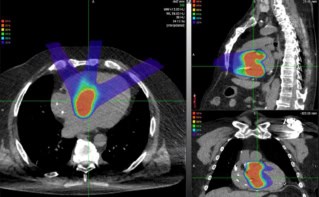
The National Physical Laboratory (NPL) has for many years supported the provision of radiotherapy in the UK, offering calibration and audit services, as well as supporting the development of world-leading codes of practice. More recently, with the introduction of advanced techniques such as intensity-modulated radiotherapy, stereotactic ablative body radiotherapy and stereotactic radiosurgery, NPL played a key role in ensuring the safe and optimized uptake of these new treatments.

NPL is now gearing up for a new challenge, as the UK launches its first high-energy proton therapy facilities. The UK was the site of the world’s first hospital-based proton therapy centre: the low-energy ocular treatment facility at Clatterbridge Cancer Centre, which started treating patients in 1989. Since then, though, the country has lagged behind in establishing a high-energy facility.
Later this year, however, the UK’s National Health Service (NHS) will open its first high-energy proton therapy centre, at The Christie, followed in 2020 by a second facility at UCLH. Both will employ the latest pencil-beam scanning beam delivery. There are also several private centres under development, such as the Rutherford Cancer Centres, which is also aiming to offer proton treatments in 2018.
“Overall, our experience with proton therapy is still much smaller than in the radiotherapy world,” said Richard Amos from University College London, speaking at the recent launch of NPL’s Metrology for Medical Physics Centre (MEMPHYS). “Having a central place like NPL to keep it on track is a great idea – this is why MEMPHYS is so important.”
Absolute dosimetry
One key service offered by NPL is absolute dosimetry of radiotherapy systems. The laboratory has developed graphite calorimeters as primary standards for measuring absorbed dose. These are used to calibrate clinical instruments that hospitals send to NPL, by comparison against the calorimetry results in one of NPL’s well defined linac facilities.
“We make sure that a patient receiving radiotherapy anywhere in the UK will receive the same radiation dose,” explained Russell Thomas, senior research and clinical scientist at NPL.
While this service ensures excellent consistency for conventional radiotherapy performed in the UK, NPL cannot repeat this model for proton therapy as it does not have an on-site proton therapy system. Previously, the only option for proton beam reference dosimetry was a 60Co-based calibration, which has an uncertainty of about 5-9%. But what’s really needed is the same level of uncertainty achieved for radiotherapy – an accuracy of nearer 2%.
“It’s really important that we can deliver proton therapy as well as we currently deliver standard radiotherapy,” said Rebecca Nutbrown, NPL’s head of metrology for medical physics, noting the importance of end-to-end audits and equipment calibration. “We aim to halve the reference dosimetry uncertainty for proton therapy from the current levels that are based on the international code.”
Proton focus
The nature of proton dose delivery – where the beam deposits most of its energy at a defined distance, within the Bragg peak – makes it of the utmost importance to perform treatments with as high an accuracy as possible. Positional uncertainty due to patient breathing, for example, and anatomical variations such as tumour shrinkage or cavity filling can change the beam range and dramatically degrade the intended dose deposition. “Proton therapy is amazingly conformal, but runs the risk of geometric miss of tumours,” Amos noted.
Much research is currently dedicated to addressing this problem, using emerging in vivo range verification techniques, for example. Meanwhile, proton CT and dual-energy CT are being studied as ways to increase treatment planning accuracy. “Accounting for all uncertainties in proton therapy planning is more complicated than photon planning; and it’s so complicated that not all sites do it the same way,” Amos explained. “Standardizing the way that we account for uncertainties is important.”
To achieve this, NPL is developing a code of practice for proton beam dosimetry, in collaboration with the Institute of Physics and Engineering in Medicine (IPEM). NPL has also established the Proton Physics Research and Implementation Group (PPRIG), with representatives from key stakeholders including The Christie and UCLH.
Another essential task is absolute dosimetry for calibration of the proton beam. With this aim, NPL is developing a primary standard for protons, based on a robust portable graphite calorimeter. This calorimeter has now been transported to proton therapy centres in Liverpool (Clatterbridge), Sicily, Prague and Japan, where it operated successfully in clinical settings.

The proton calorimeter will ultimately provide traceability that is comparable with existing UK dosimetry protocols for conventional X-ray radiotherapy. The improved consistency provided will be of benefit for multi-centre clinical trials. “With more proton centres starting up, we want them all doing the same thing, so we can glean the best knowledge with regard to treating patients,” said Thomas. “This calorimeter will become the UK’s primary standard for protons, but there’s work to do still.”
Looking forward, NPL will play a vital role in the introduction of the UK’s proton therapy centres, including performing absolute and relative dosimetry, and standardization of clinical trials and imaging protocols. NPL-led research will endeavour to understand uncertainties in more depth, as well as investigate radiobiology problems, such as the correlation between LET and RBE. “MEMPHYS is bringing the physical sciences together with the life sciences,” Amos concluded.