The use of PET scans to confirm the presence of dementia-inducing amyloid plaque in the brain may be ready for routine clinical use, based on a prospective study published in JAMA Neurology. Researchers found that both positive and negative results influenced the diagnosis and treatment of patients with and without dementia (JAMA Neurol. 10.1001/jamaneurol.2018.1346).
The researchers took the unique approach of enrolling subjects ranging from patients with confirmed cognitive impairment to people with no dementia at all. They discovered the presence of amyloid in both sets of subjects, which could provide a “bridge between validating amyloid PET in a research setting and implementing this diagnostic tool in daily clinical practice,” they wrote.
“Our findings demonstrate that both amyloid-positive and amyloid-negative PET results changed diagnosis and treatment in a significant number of patients,” said lead author Arno de Wilde from VU University Medical Center (VUMC) in Amsterdam. “We observed this in both patients with and without dementia, [so] amyloid PET can be of value in a selection of patients in clinical practice.”
Amyloid factor
The accumulation of beta amyloid in the brain is one key indicator of possible progression to dementia or Alzheimer’s disease. With the development of tracers such as carbon-11-labelled Pittsburgh Compound B (C-11 PiB) and amyloid PET imaging, the modality has become increasingly important in the research of neurodegeneration.

Researchers at VUMC have been performing amyloid PET scans in selected research patient populations for several years now. More recently, they have begun to make the modality available in clinical practice, using amyloid PET in people seen in the institution’s memory clinic as part of routine diagnostic workup, de Wilde wrote in an email to AuntMinnie.com.
“We offered amyloid PET to all patients visiting our clinic, even if they were not cognitively impaired or there was no suspicion of Alzheimer’s disease,” he said. “This unique approach gave us the opportunity to determine the value of amyloid PET in an unselected memory clinic population.”
VUMC’s amyloid PET protocol includes the radiotracer florbetaben (Neuraceq, Piramal Imaging). It is indicated for PET imaging to estimate beta-amyloid neuritic plaque density in adult patients with cognitive impairment who are being evaluated for Alzheimer’s disease and other causes of cognitive decline.
Florbetaben is one of three F-18-labelled amyloid PET tracers that have been approved by the US Food and Drug Administration and the European Medicines Agency for clinical use. The other two are florbetapir (Amyvid, Eli Lilly) and flutemetamol (Vizamyl, GE Healthcare).
“Amyloid PET has been proven to be a valid and stable technique to visualize cerebral amyloid plaques,” de Wilde said. “However, studies that demonstrate the usefulness of amyloid PET in patients whose diagnosis and treatment are based on amyloid PET status are lacking.”
Clinical subjects
The researchers enrolled 507 patients from VUMC’s memory clinic who were participating in the Alzheimer Biomarkers in Daily Practice (ABIDE) project between January 2015 and December 2016. The subjects had a mean age of 65 years (±8 years) and varying degrees of dementia and cognitive issues.
The subjects consisted of 164 (32%) people with Alzheimer’s dementia, 114 (23%) with mild cognitive impairment, 159 (31%) with subjective cognitive decline, and 70 (14%) with non-Alzheimer’s dementia. Cognition evaluations were based in part on Mini-Mental State Examination (MMSE) test scores and a family history of dementia.
From that information, one of two neurologists who co-authored the study determined whether subjects presented with clinical symptoms of Alzheimer’s, such as dementia, mild cognitive impairment or subjective cognitive decline. The neurologists then determined the suspected aetiology of the symptoms, with causes including Alzheimer’s disease, vascular problems, frontotemporal dementia, Lewy body dementia or a neurodegenerative disease. The physicians then rated their level of diagnostic confidence in the suspected aetiology on a scale of 0% to 100%.
Amyloid accumulation
The researchers found evidence of amyloid on the PET scans of 242 patients (48%). Amyloid was most prevalent among the 164 patients with Alzheimer’s dementia: 128 were amyloid-positive (78%). Subjects with non-Alzheimer’s dementia were the next most prevalent group, with 45 (64%) of 70 being positive for amyloid.
After undergoing amyloid PET scans, the suspected aetiology changed for 125 patients (25%), with a negative PET scan contributing more significantly to the change in diagnosis than a positive PET scan.
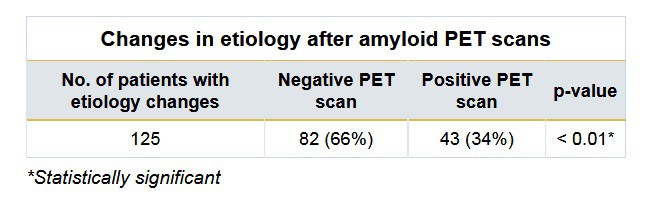

Treatment plans changed for 123 patients (24%), the researchers found. A positive amyloid PET scan prompted changes in medication, a clinical trial referral or both, while a negative amyloid PET scan most often resulted in a follow-up FDG-PET scan, genetic screening or referral to a psychiatrist.
Changes in diagnoses did not differ significantly between patients with dementia (50 of 234, 21%) versus subjects without dementia (75 of 273, 28%) (p > 0.05).
As for the neurologists reading the results, the additional information gleaned from the amyloid PET scans boosted their diagnostic confidence by a mean of 80% to 89% (p < 0.001).
“This study goes beyond previous findings, as we also assessed patient-reported outcomes,” the authors wrote. “More than 80% of patients experienced the PET scan as not burdensome. One-fifth of patients expected the PET scan to be burdensome, and a similar fraction, looking back, said to have experienced the PET scan as burdensome.”
In addition, when patients were told of the amyloid PET scan results, their level of uncertainty decreased while their anxiety levels remained stable. That finding, de Wilde suggested, means that disclosing the PET result in clinical practice does not have an adverse effect on patients’ psyche.
“The current study demonstrates that amyloid PET can be valuable in a selection of patients,” he concluded. “We are currently trying to identify those patients who benefit most from amyloid imaging and create a tool that helps clinicians to identify those patients.”
- This article was originally published on AuntMinnieEurope.com © 2018 by AuntMinnieEurope.com. Any copying, republication or redistribution of AuntMinnieEurope.com content is expressly prohibited without the prior written consent of AuntMinnieEurope.com