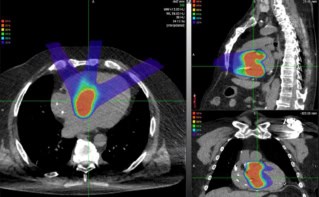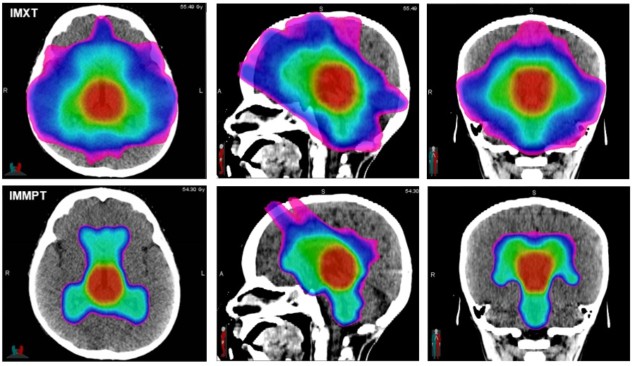
A team at St. Jude Children’s Research Hospital has developed and validated a new intensity-modulated minibeam proton therapy (IMMPT) system. The system is designed to improve high-dose conformity at mid-depths compared with current pencil-beam scanning proton therapy systems. It may be able to improve treatments for brain tumours by delivering more precisely targeted radiation and reducing dose to surrounding normal tissues (Med. Phys. 10.1002/mp.13093).
Intensity-modulated proton therapy (IMPT) systems utilize individual beamlets that have optimized intensities to provide a balance between target dose and dose to normal tissues. They offer improved efficiency, proximal dose sparing and flexible applications compared with legacy double-scattering delivery systems. Improvements have reduced spot sizes to around 3 mm.
To reduce spot sizes further, field collimation is being utilized to improve target conformity and penumbra, the region at the edges of a radiation beam where a rapid dose reduction occurs. To simplify this process, the research team, led by Jonathan Brent Farr, aimed to create a system that produces much smaller clinical proton beamlets without the need for physical collimation.
Farr and colleagues modified a proton therapy system in regular clinical use in the hospital’s Red Frog Events Proton Therapy Center. They made two modifications to the system’s fixed horizontal beamline – adding and activating a vertical scraper to achieve a smaller beam size extracted from the synchrotron, and adopting a thinner vacuum window at the end of the beam line in the scanning nozzle – to enable IMMPT delivery using scanned minibeams. They also improved the proton spot position monitor and patient positioner accuracy to support clinical IMMPT delivery.
The researchers performed integral depth dose (IDD) acquisitions and calibrations, and compared IDDs, spot profiles and transmission chamber energy calibration curves with those from the regular system. They developed and validated Monte Carlo models and used these to produce spot profiles and IDDs. These were then imported into a commercial treatment planning system for dose model fitting, testing and validation.
Two patient plans were developed for a simulated base-of-skull case with small and medium targets proximal to the brainstem: one using a nominal discreet spot-scanning system and the other using the minibeam. The team compared these using dose difference and dose volume histogram analysis. The minibeam patient plan was also evaluated using the department’s standard patient-specific quality assurance programme.
The authors reported that the differences between 96 IDD measurements for the minibeam treatment compared with the standard spot commissioning data were indistinguishable. “The spot sigma is determined to be 1.4 mm at 221 MeV at the isocentre and below 1 mm at proximal distances,” they wrote, adding that “the treatment planning system [data] fit the spot profiles closely, giving a residual error maximum of 2.5% in the spot penumbra tails from 69.4 to 221.3 MeV.”
The resulting IMMPT plans delivered superior target conformity and brainstem sparing for both the small and medium targets. The authors attributed this to a steeper dose gradient compared with IMPT.
Farr tells Physics World that the IMMPT system has received 510(k) clearance from the US Food and Drug Administration and is in routine clinical use at St. Jude. “Currently, the physician-scientists are using the superior dose sparing properties of the minibeam to enhance the care of children with relatively small brain tumours abutting critical structures like the brain stem and optic nerves,” he says.
“An upcoming investigation using the IMMPT system to treat a range of ocular tumours is under development. Here, the additional sparing properties of the minibeam may be used to preserve orbital bone growth for the affected children,” he adds.
Farr, currently director of medical physics at Advanced Oncotherapy, a proton therapy system company headquartered in London, believes that the clinical use of proton minibeams will increase over time. He and his colleagues at Advanced Oncotherapy are working to investigate and develop proton minibeams to yet higher conformity.