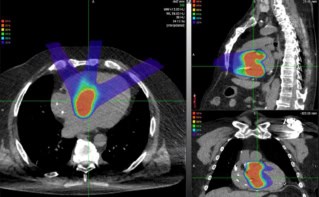
In vivo monitoring of beam range and applied dose is a key enabler for precision particle therapy delivery. One approach under investigation is PET imaging of positron emitters generated during treatment. But for accurate treatment verification, correction of biological washout is essential.
PET verification of particle therapy (proton and carbon ion) works by imaging positron emitters – mainly 11C and 15O – produced along the beam path as the beam interacts with tissues in the patient. The resulting PET images can then be compared with a calculated reference activity distribution. In living objects, however, diffusion of the positron emitters causes biological washout of activity, which can significantly affect the spatial distribution of the PET signal.
For in-beam and in-room PET, 15O is the prevalent contributor, due to its relatively short half-life of 2.03 min. For off-line PET (performed after treatment), 11C – with a half-life of 20.39 min – dominates. Current biological washout models were developed based on animal studies of 11C beams. But such models might not be suitable for early time frames, as washout of 15O and 11C ions may behave differently.
To provide more accurate modelling of 15O biological washout, a research team from Tokyo Women’s Medical University and the National Institute of Radiological Sciences measured the washout rates of 10C, 11C and 15O ion beams in the rabbit brain. They employed the whole-body dual-ring OpenPET, a full-ring in-beam PET system that acquires data during pauses in pulsed beam delivery and immediately after irradiation (Biomed. Phys. Eng. Express 4 035001).
Radioactive beams
PET verification of patient treatments employs the positron emitters generated by the proton beam. However, this is a weak effect, so for this study the team employed radioactive beams of positron-emitters, generated as secondary beams in the Heavy Ion Medical Accelerator in Chiba (HIMAC).
“The precision of autoactivation imaging is low due to poor statics of the positron emitting nuclides generated during irradiation,” explained first author Chie Toramatsu. “Using a radioactive primary beam overcomes the problem.”
The researchers irradiated the brains of three anaesthetized rabbits with 10C and 11C beams, starting PET imaging simultaneously with the start of irradiation. They performed measurements using the OpenPET prototype, which comprises two 660-mm diameter detector rings, with the animal placed in the 90 mm gap between the rings.
First, the team delivered 3×20 spills of 10C to the target, followed a few minutes later by three spills of 11C (this was possible due to 10C’s very short half-life of 19.2 s). They performed PET for 200 s for the 10C and 40 min for the 11C beam. Subsequently, the rabbit was sacrificed, and after 120 min, re-irradiated with 10C and 11C beams in the absence of biological effects.
Three other rabbits were irradiated with three spills of 15O, and imaged for 20 min. The experiment in the dead condition was performed immediately afterwards.
PET images summed over 0-150, 0-2400 and 0-600 s (for 10C, 11C and 15O, respectively) revealed that the PET intensity in the region-of-interest (ROI) was significantly lower in the live animals. This was due to the washout effect and was observed for all three irradiation types.
Washout model
To analyse the washout effect, the researchers generated time activity curves (TACs) from the acquired PET data divided into 30 s frames. They used multiple component model analysis to obtain the washout rates from these TACs.

Plotting ROI activity (in arbitrary unit) versus time demonstrated that, due to the washout effect, ROIs values decreased faster in the live animals. The researchers note that 15O and 11C ions exhibited different biological decay behaviours, with the washout rate of the 15O beam significantly larger than that of the 11C beam.
For 10C and 11C, the TACs of the ROIs fitted well to three exponential functions. The observed washout rates of these fast, medium and slow components were 21.04, 0.34 and 0.004 min-1, respectively. These values are consistent with previous rat and rabbit studies. For 15O, TACs fitted well to two exponential functions, with medium and slow biological decay rates of 0.72 and 0.024 min-1, respectively.
To integrate PET-based dose verification into particle therapy, in-room and in-beam PET are likely the optimal approaches, as short-lived nuclides such as 15O are still abundant and the overall signal intensity will be significantly higher. The authors note that to employ such a setup clinically, modelling biological washout for 15O is essential for correct prediction of activity distributions, and suggest that the 15O washout rate obtained in this study is applied. They add that the long-term aim is to establish an appropriate washout model, for both washout correction and to guide adaptive therapy.
“The washout effect can be used to monitor tumour tissue changes due to irradiation in real-time,” Toramatsu explained. “For example, the washout rate might be slower and the signal intensity lower in necrotic tumour because of poor vascularization and hypoxia; this means that higher dose should be delivered.”
The team is now examining the chemical reactions between tissue elements and positron emitters to understand the biological effects that are reflected in the washout.