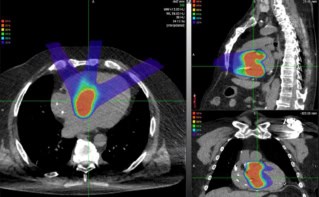
Children with cancer are arguably set to benefit most from proton therapy as the number of clinics worldwide continues to grow. Steep dose gradients enable superior sparing of healthy tissue compared to photons, reducing the lifetime risk of radiation-induced cancer and increasing survival.
The majority of paediatric patients, however, do not have access proton therapy. Aside from a handful of centres in China and Russia, no low- to middle-income countries have operational proton clinics.
“Eighty per cent of children live in developing countries and they’re not receiving the most effective and safe radiotherapy possible,” says Phillip Taddei, a medical physicist at the University of Washington in Seattle. “We need to change that.”
An American-Lebanese collaboration led by Taddei has compared the projected lifetime risk of radiation-induced cancer at specific anatomical sites and mortality in paediatric medulloblastoma patients receiving proton or photon therapy. The researchers estimate that more than 1000 lives could be saved annually with global access to proton therapy (Biomed. Phys. Eng. Express 4 025029).
The in silico clinical trial is part of a larger effort by the collaboration to demonstrate measurable differences in outcomes for children receiving proton therapy instead of photon-based treatments. Supported by a Fogarty International Center award, Taddei worked on the study while based at the University of Texas MD Anderson Cancer Center in Houston and the American University of Beirut Medical Center.
Lower the risks
The collaboration compared the risks from proton and photon therapy in five girls and four boys aged two to 14, preparing proton and photon plans for each child. Each had already received proton therapy in Houston.
Craniospinal irradiation (CSI) proton plans using passive-scattering spread-out beams were prepared according to protocols at MD Anderson. Photon plans were prepared using conventional 3D conformal radiotherapy according to routine practise at the American University of Beirut.
Treatment planning systems at each centre calculated the mean equivalent dose received by each organ and tissue types at risk of radiogenic cancer, such as the lungs and breast tissue. Out-of-field dose contributions were calculated using separate models.
The researchers used the doses to estimate the lifetime attributable risk of secondary cancer for each anatomical site and the associated mortality. The site-specific risks of solid tumours were calculated with a linear no-threshold model. The total lifetime risk was calculated by summing the risks over all sites.
Rather than examine absolute risks, the collaboration calculated ratios of the risks due to proton therapy compared to photon therapy. As relative measures, the ratios are subject to significantly lower uncertainty.

Absolute risks of radiogenic cancer incidence and death were revealed to be high for both treatment modalities, but substantial reductions were demonstrated using protons. The overall risk of secondary cancer was reduced by 44%, while mortality was reduced by 36%.
“In particular, we found for fatal site-specific secondary cancers, that proton therapy was most advantageous for reducing subsequent lung, colon and breast cancer,” said Taddei. Overall, the authors estimate that roughly 1010 deaths each year and 48,000 deaths over thirty years could be prevented if children in developing countries had access to proton therapy.
In a separate study still in progress, the collaboration is assessing the benefits of proton therapy in children with intra-cranial brain tumours. Further studies of other paediatric tumours routinely treated with radiotherapy are planned.
Centralized centres
Looking ahead, the authors identify regional, centralized proton clinics with large, international population catchments as the most promising way to reduce the risks for paediatric patients in low- to middle-income countries.
Obstacles such as up-front cost, infrastructure, training and international cooperation are significant, but surmountable, according to Taddei. Philanthropy, for example, is already being used to fund new facilities at the American University of Beirut.
“In the developing countries of the Middle East, centralized care is [also] already a reality,” Taddei told medicalphysicsweb. The Children’s Cancer Centre of Lebanon in Beirut, for instance, already treats children from Syria and Iraq with photon-based radiotherapy without charge to the families.